Bart Decadt
Consultant Laparoscopic Bariatric
& Upper GI Surgeon







Gastric Bypass
How is the Gastric Bypass performed?
Gastric Bypass surgery (the Roux-en-Y Gastric Bypass) is usually performed under general anaesthesia using keyhole (laparoscopic) surgery. Small incisions are created in the abdominal wall to allow small instruments to be passed into the abdominal cavity, guided by a special surgical telescope with a video camera, in order to perform the operation.
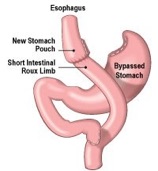
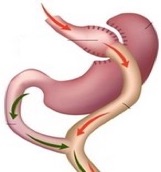
Using surgical staples the surgeon will create a small pouch from the upper stomach, partitioning it from the lower part of your stomach. The stomach pouch is then connected directly to the middle portion of the small intestine (jejunum), bypassing the rest of the stomach and the upper portion of the small intestine (duodenum). Very rarely a drain is inserted to stop fluid from collecting inside your abdomen
Dr Bart Decadt also has expertise with the mini-Gastric Bypass operation in which the intestine is not divided but is linked to the small gastric pouch where 150-200cm of the jejunum is bypassed. This procedure is simpler than the Roux-en-Y Gastric Bypass and therefore might have lower complication rate, but offers weight loss comparable to the Roux-en-Y Gastric Bypass. However, there is a small risk of troublesome bile reflux that could be difficult to treat and might require laparoscopic conversion to Roux-en-Y Gastric Bypass in approximately 1% of patients.
How does the Gastric Bypass work?
In addition to reducing the capacity of the stomach, which restricts the amount you can eat and reduces your appetite, Gastric Bypass surgery reduces calorie absorption as food bypasses the rest of the stomach and the upper part of the small intestine. It also causes dumping syndrome (feeling dizzy and lightheaded if you eat too much carbohydrates or sweets due to food high in sugar passes quickly from the stomach pouch into the remaining small intestine) that will deter from food over-indulgence.
How long will I stay in hospital after the surgery?
Most patients will be able to go home the following evening after surgery, and some 20% will stay an additional night or perhaps two depending on their health issues, especially their mobility, and availability of support at home.
Who is suitable for Gastric Bypass surgery?
Gastric Bypass surgery is recommended for the following groups of people:
When appropriate non-surgical measures have been tried but failed to achieve or maintain adequate, clinically beneficial weight loss in patients whose BMI is 40 kg/m2 or more Or between 35-40 kg/m2 in association with other significant disease (for example, type 2 diabetes, heart disease or high blood pressure)
It is also recommended as a first-line option (instead of lifestyle interventions or drug treatment) for adults with a BMI of more than 50 kg/m2 in whom surgical intervention is considered appropriate (National Institute for Clinical Excellence).
In March 2011, The International Diabetes Federation (IDF) recommended bariatric surgery to patients with BMI 30 kg/m2 (Asians from BMI 27.5 kg/m2) if their diabetes was poorly controlled. Gastric Bypass operation is particularly useful for those who crave for sweets (sweet-eaters)
However, the need for surgery to aid weight loss and the choice of surgical procedure is dependent on discussion with the bariatric team who will provide you expert and comprehensive advice.
What are the benefits of Gastric Bypass surgery?
Considerable and durable weight loss up to 65-75% of excess body weight within 12-18 months. Marked improvement or resolution in health conditions related to obesity, particularly type-2 diabetes (approximately 80-85% chance of resolution), hypertension (60-75% chance of resolution) gastro-oesophageal reflux, obstructive sleep apnoea (90% chance of resolution), asthma, polycystic ovary syndrome (PCOS) and associated infertility, liver disease, high cholesterol, and painful osteoarthritis. Improvement in overall physical and psychological health
What are the risks of Gastric Bypass surgery?
As with any surgical operations there are associated short and long-term complications such as internal bleeding, anastomosis Leakage, blood clot in the legs (deep vein thrombosis; DVT), blood clot in the lung (pulmonary embolism), infection, malabsorption of vitamins and micronutrients (which may lead to anaemia, weakness, osteoporosis and neurological problems), internal bowel hernia (less than 1%), ulcer perforation (0.8%), and weight regain.
However, Dr Decadt has performed over 1600 Gastric Bypass procedures with results that are amongst the best when compared to the World’s experience. In particular, he has not needed to convert any to an open operation. His procedure-related risk to life was 1-in-550 (0.15%) compared to a World average of 1-in-100 (1%).
His anastomosis leak rate is 1-in-400 (0.25%) compared with a World average of 1-in-200 (0.5%). The joint between the stomach and intestine is hand-sewn to reduce the risk of leak and is then tested at the end of surgery with a blue dye to ensure “no leak” but until that joint heals (takes usually 2-3 weeks), you’ve got to stay on liquid diet and take acid-lowering tablets to prevent an ulcer at that joint.
To prevent clots in the legs, we advise that you keep the elastic stockings we give you and to take the heparin injections for few days (occasionally for up to 4 weeks) after leaving the hospital. This is why perhaps only three patients in our experience have had clots after surgery.
It is also essential to take the recommended iron-calcium and supplements multivitamin (including vitamin D and 3-monthly injections of vitamin B12) long-term and to have blood tests every year to check on these.
Will I regain the weight?
Although the weight loss is durable, 1-in-10 people might regain the weight within 10 years of surgery. The stomach could stretch, the hunger could return, the intestine adapts and the dumping fades away. It is essential therefore to adopt a new life style and carry it on for a durable result.


Contact Private Secretary (Barbara Dawson)
Telephone 0161 440 9997 Fax 0161 440 8818 Mobile 07802 445558


CALCULATE YOUR BMI
THE PATIENT JOURNEY

All Enquiries
0161 440 9997

































request a quote
to request a quote or a call to discuss your surgical needs






to go to the NBSR website


“I enjoy attending the monthly support group sessions where I am helped by others who have experienced weight loss surgery..”






MBS (Manchester Bariatric Services)






